When Distance Became the Disease: How Telehealth and AI are Transforming Healthcare Access in Nepal
In early 2020, as the COVID-19 pandemic swept across the world, healthcare systems everywhere were pushed to their limits. Hospitals closed their doors to non-emergency care, movement was restricted, and for many people, seeing a doctor became suddenly impossible.
In Nepal, where geography already stands between communities and healthcare, the disruption was even more profound.
Out of this crisis, telehealth quietly emerged as a lifeline.
Using something as simple as a mobile phone, an internet connection, and a trained health worker with portable diagnostic tools, care could travel where patients could not. Screening, consultation, referral, and follow-up no longer had to begin with a long journey to a city hospital. Instead, healthcare could reach people where they lived.
For communities scattered across hills, plains, and remote villages, telehealth was not a convenience – it was access.
Bringing Specialists Closer to Home
Nepal’s healthcare system has long struggled with uneven distribution of specialist services. Eye care and ENT services, in particular, are often concentrated in urban centers, leaving rural populations with few realistic options. Travel is expensive, time-consuming, and sometimes physically impossible for elderly patients, people with disabilities, or those living in extreme poverty.
Telehealth helped bridge this gap.
Patients could now receive consultations, basic examinations, and referrals without leaving their communities. Trained health workers equipped with portable diagnostic tools became the first point of care, connecting patients to specialists at base hospitals. This shift reduced patient burden, encouraged earlier health-seeking behavior, and strengthened primary-level care.
Recognizing this potential, CHEERS initiated tele-ophthalmology and tele-otology services in 2020, starting at community outreach centers within Kathmandu Valley. The Ophthalmic Assistants and BPEF-CHEERS trained Community Ear Health Workers were then deployed at satellite centers equipped with digital slit lamps, portable fundus cameras, tonometers, digital otoscopes, laptops, and reliable internet connections. Through tele-consultation platforms developed in-house at CHEERS, these frontline workers could connect directly with ophthalmologists and ENT specialists at the base hospital. Complex cases were discussed remotely, medical images were shared, and treatment plans were guided in real time.
For patients, this meant fewer journeys, lower costs, and faster care.
For health workers, it meant confidence, mentorship, and professional growth.
A Diagnosis Caught in Time
The impact of this model is best understood through the example of Sita Prajapati, a 52-year-old woman from Lele Village in Lalitpur District.
She attended a free Daily Screening and Treatment Service (DSTS) camp organized by CHEERS, believing that her mild vision problem could be corrected with glasses. She had diabetes but had not been taking medication regularly and had no alarming symptoms.
During routine screening, a fundus photograph taken by an ophthalmic assistant revealed something far more serious: proliferative diabetic retinopathy, a condition that can silently steal vision if left untreated.
Within moments, Sita was connected virtually to an ophthalmologist at the CHEERS base hospital. What could have been missed was caught in time. Today, she is under regular follow-up with a retina specialist and has already undergone two sessions of retinal laser treatment – her vision preserved because care reached her early.
Extending the Same Care to Remote Areas
In 2021, BPEF-CHEERS expanded this approach to Purvanchal Eye, ENT, and Rehabilitation Services in Ratuwamai, Morang and another Community Eye , ENT and Rehabilitation Center (CEERC), in Adarsha Kotwal, Bara.
Community Ear Health Workers (CEHWs) were trained to use digital otoscopes to examine patients for middle-ear diseases. Through secure web-based platforms, they shared images and conducted real-time virtual consultations with ENT specialists. Conditions that once went undiagnosed, or untreated until complications arose, were now being identified early. For many patients, this was the first time ear care felt accessible, understandable, and trustworthy.
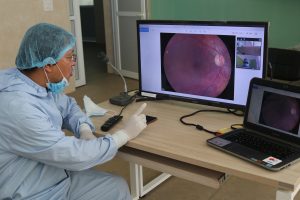
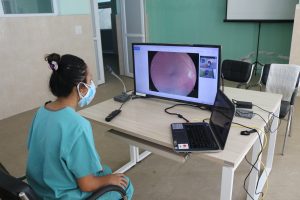
When Telehealth Alone Was Not Enough
As telehealth services expanded, so did their challenges.
Outreach programs were limited by the availability of specialists at tertiary centers. Every case required expert review. Patient waiting times grew. Scaling services meant stretching already scarce human resources even thinner. Subtle early-stage diseases – especially in eyes and ears – were still at risk of being missed.
It became clear that telehealth needed reinforcement.
To address these limitations, CHEERS began developing Artificial Intelligence (AI) -augmented telehealth systems, supported by funding from Direct Relief under the “CHEERS Telemedicine Project”.
The goal was not to replace clinicians – but to support them.
AI was designed to act as a first-level screening and triage tool, helping community health workers:
- Flag high-risk cases early
- Prioritize patients requiring urgent specialist attention
- Reduce missed or delayed diagnoses
This approach could especially be powerful in high-volume outreach settings, where early detection can mean the difference between reversible and irreversible disease.
Building AI for Local Health Needs
BPEF-CHEERS is committed to building AI that works locally, for local populations, and on existing devices that can be easily used.
Public datasets – often collected in high-income countries – do not adequately reflect Nepal’s population, disease patterns, or imaging devices. Recognizing this, CHEERS invested heavily in collecting and annotating locally sourced clinical data, using the same portable equipment deployed in rural outreach centers.
Under the Telehealth and AI Center, AI development is progressing in four key areas:
(i) AI-Augmented Tele-Ophthalmology
Eye disease remains a major public health challenge in Nepal. According to the nationwide Rapid Assessment of Avoidable Blindness (RAAB) survey disseminated by the Ministry of Health and Population in 2024, the age-sex weighted national prevalence of blindness (PVA <3/60) stands at 1.1%, while 20.7% of the population lives with some form of vision impairment. Women bear a disproportionate burden, and provinces such as Lumbini and Madhesh – where CHEERS actively works – show higher prevalence rates.
While cataract remains the leading cause of blindness, the RAAB survey highlights the growing contribution of posterior segment diseases, including glaucoma (5.8%) and age-related macular degeneration (5.3%), conditions that are often asymptomatic in early stages and easily missed without specialized screening.
Recognizing this shift, CHEERS prioritized AI development in retinal disease screening, focusing on diabetic retinopathy, glaucoma, and AMD. Thousands of retinal images have been collected using portable fundus cameras in outreach settings and annotated by multiple ophthalmologists to ensure diagnostic accuracy.
AI models initially trained on public datasets are in the process of fine-tuning using this locally generated data, improving performance in real-world Nepali clinical context. Feasibility testing for AI-assisted glaucoma screening has been conducted by integrating AI tools into routine clinical workflows at outreach centers, supporting ophthalmic assistants in identifying high-risk patients early and enabling timely referral to specialists.


(ii) AI-Augmented Tele-Otology
Middle-ear disorders are highly prevalent in Nepal, particularly among children and young adults, and remain a major cause of preventable hearing loss. Conditions such as acute otitis media (AOM), chronic otitis media (COM), and otitis media with effusion (OME) often go undetected or untreated due to limited access to ENT specialists, especially in rural and underserved areas.
To address this gap, CHEERS is developing AI-integrated tele-otology tools that analyze images captured through digital otoscopes used by Community Ear Health Workers. The AI system is embedded directly into the screening workflow and functions in a stepwise manner:
- Image gradability assessment: The AI first evaluates whether the otoscopic image is of sufficient quality for clinical interpretation. If the image is ungradable, the system prompts the health worker to recapture the image, improving data quality at the point of care.
- Automated disease prediction: Once an image is deemed gradable, the AI model analyzes it for features suggestive of AOM, COM, and OME.
- Referral decision support: Based on the AI output, the system provides referral recommendations, helping frontline workers prioritize cases that require urgent ENT consultation through telehealth or in-person referral.
By supporting health workers in acquiring high-quality images, identifying middle-ear pathology early, and guiding timely referrals, AI-augmented tele-otology strengthens early detection, reduces missed diagnoses, and helps prevent progression to chronic disease and permanent hearing impairment.
(iii) Down-Syndrome Screening
Early identification of Down syndrome remains limited in many low-resource settings in Nepal, particularly in rural areas where access to pediatric specialists and diagnostic services is scarce. Delayed identification often results in missed opportunities for early intervention, rehabilitation, and timely family counseling.
To address this gap, CHEERS has been developing a mobile app-based AI screening tool designed to support early risk identification at the community level. The application assists frontline health workers by analyzing key visual and developmental features to flag children who may require further clinical assessment.
By enabling early recognition and prompting timely referral to appropriate health facilities, the application helps families access confirmatory testing and supportive services earlier in the child’s life.
(iv) OPMD & Oral Cancer Screening
Oral potentially malignant disorders (OPMD) and oral cancer represent a growing public health concern in Nepal, particularly among populations with high tobacco and alcohol use. Late presentation remains common, contributing to poor treatment outcomes and high mortality.
CHEERS has developed an AI screening tool based on a mobile app that analyzes intra-oral images captured on mobile devices during community outreach and screening programs. The application supports frontline health workers in identifying suspicious oral lesions that may indicate OPMD or early-stage oral cancer.
The tool serves as an early screening and risk-flagging system, helping health workers identify individuals who require further clinical evaluation or referral. By shifting detection earlier to more treatable stages, this approach aims to reduce delayed diagnosis and improve oral cancer outcomes in underserved communities.
Looking Ahead
With over 3,000 tele-consultations conducted, more than half of the beneficiaries were women, and a significant proportion were children and older adults.
What began as a response to a global crisis has grown into a vision for the future of healthcare in Nepal – one where distance is no longer a diagnosis, and where technology strengthens, rather than replaces, human care.
With continued support from partners like Direct Relief, CHEERS is not just delivering telehealth – it is building a system where early detection, equity, and dignity are part of everyday care.
Learn more about the platforms and AI systems in use at: https://cheersai.org
References
Shakya, M., Adhikari, B., Shrestha, N., Koirala, B., Adhikari, A., Poudyal, P., Mathema, L., Buddhacharya, S., Khatri, B., & Khanal, B. (2025). From development to deployment of AI‑assisted telehealth and screening for vision‑ and hearing‑threatening diseases in resource‑constrained settings: Field observations, challenges and way forward (arXiv:2509.15558). arXiv. https://arxiv.org/abs/2509.15558
Mishra, S. K., Shah, R., Gogate, P., Sapkota, Y. D., Gurung, R., Shrestha, M. K., Mactaggart, I., Shahi, B. B., & Burton, M. (2025). Prevalence and causes of blindness and vision impairment among people 50 years and older in Nepal: A national Rapid Assessment of Avoidable Blindness survey. PLOS ONE, 20(2), e0309037. https://doi.org/10.1371/journal.pone.0309037
Mathema, L., Shrestha, R., Adhikari, A., Poudyal, P., Upadhyay, S. K., & Khatri, B. (2022). Acceptability and feasibility of community management of ear patients through tele‑otology services in outskirts of Kathmandu Valley, Nepal. MedS Alliance Journal of Medicine and Medical Sciences, 2(3), 12–17. https://doi.org/10.3126/mjmms.v2i3.47655